Trauma and the Brain
During highly stressful events, the brain and body undergo a series of physiological changes that prepare the individual to safely escape or respond to the danger.
The Brain During Highly Stressful Situations.
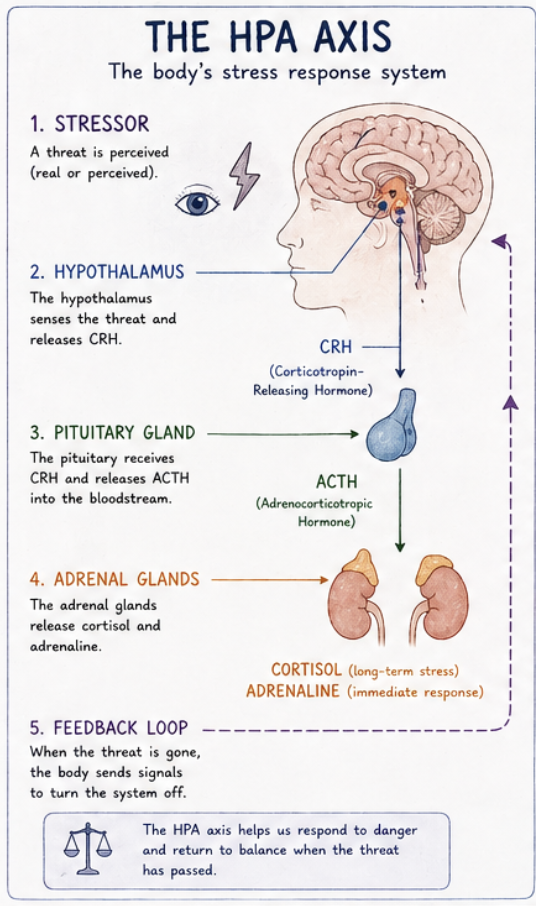
Importantly, in a typical, non-traumatic stress response, this system is both proportional and temporary. Once the threat has passed, the body engages a self-regulating mechanism known as a negative feedback loop, in which rising cortisol levels signal the brain to reduce and eventually stop the stress response. This allows the nervous system to return to baseline, restoring balance and enabling higher-level cognitive processes to come back online. At that point, the individual can reflect on what happened, integrate the experience, and store it as a coherent memory. In this way, the stress response is not harmful in itself, it is an essential biological system that allows humans to respond quickly to danger while still maintaining the capacity for recovery, learning, and adaptation afterward.
When the brain and body encounter a threatening situation, they activate a highly coordinated and adaptive survival system designed to protect the individual. This process begins in the limbic system, particularly the amygdala, which rapidly detects potential danger and sends signals to initiate the body’s stress response. In milliseconds, the hypothalamic-pituitary-adrenal (HPA) axis is activated, releasing stress hormones such as adrenaline, norepinephrine, and cortisol into the bloodstream. These hormones prepare the body for action by increasing heart rate, sharpening attention, redirecting blood flow to major muscle groups, and slowing non-essential processes like digestion. This immediate, automatic response, often referred to as the “fight, flight, or freeze” response, occurs largely outside of conscious awareness and prioritizes speed over accuracy in order to maximize chances of survival. During this time, information is processed along a rapid “low road,” meaning it may bypass higher-order brain regions like the prefrontal cortex, which are responsible for reasoning and reflection.
Dysfunction of Stress Response
When this system becomes dysregulated, the same mechanisms that are designed to protect the individual can begin to work against them. Instead of activating only in the presence of real and immediate danger, the stress response may become hypersensitive, overactive, or difficult to turn off. The brain continues to detect threat even in relatively safe environments, and the body remains in a prolonged state of physiological arousal
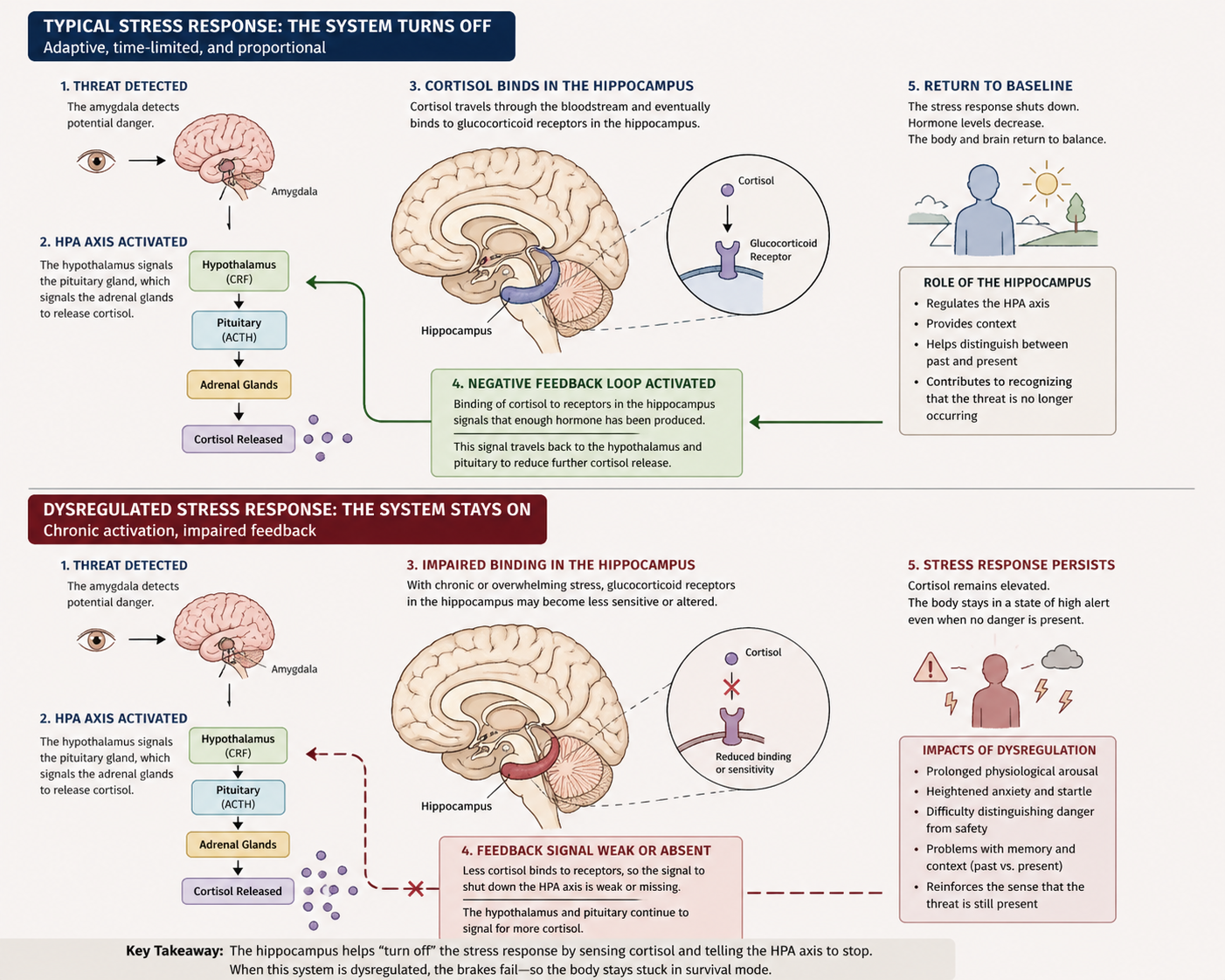
A key structure involved in “turning off” the stress response is the hippocampus, which plays a critical role in both memory and regulation of the HPA axis. Under typical conditions, as cortisol is released during a stress response, it eventually binds to glucocorticoid receptors in the hippocampus. This binding acts as a signal that enough stress hormone has been produced, initiating a negative feedback loop that suppresses further activation of the HPA axis and allows the body to return to baseline. In addition to this regulatory role, the hippocampus helps provide context, distinguishing between past and present, and contributes to recognizing when a threat is no longer occurring. However, when this system becomes dysregulated, as can occur with chronic or overwhelming stress, the sensitivity and functioning of these receptors may be altered. Cortisol may no longer bind as effectively, weakening the feedback signal that typically shuts the system down. As a result, the stress response can persist even in the absence of real danger, with continued hormone release and ongoing physiological arousal. This disruption not only prolongs the body’s survival response but also contributes to difficulties in accurately contextualizing experiences, reinforcing the sense that the threat is still present even when it has passed.
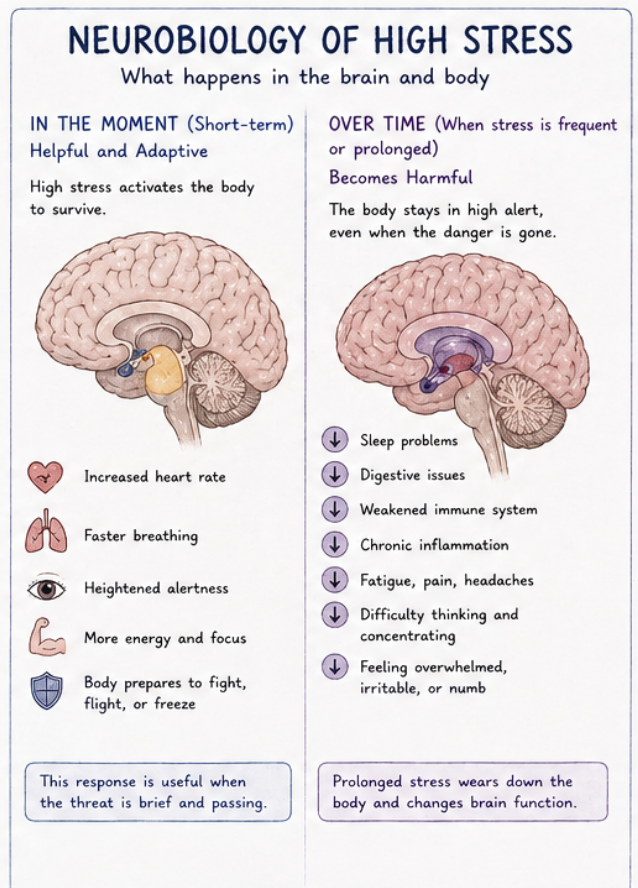
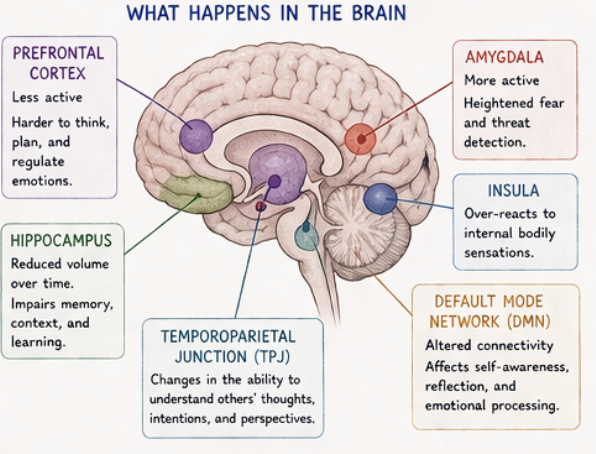
As a result, neural processing shifts further away from higher-order brain regions and becomes increasingly dominated by the limbic system. The amygdala becomes more reactive, amplifying fear and threat detection, while the prefrontal cortex becomes less effective in regulating emotional responses and distinguishing between real and perceived danger. This imbalance makes it more difficult for individuals to accurately interpret their environment, as neutral or ambiguous stimuli may be experienced as threatening.
Over time, this chronic activation reinforces neural pathways associated with survival, making these responses more automatic and more difficult to interrupt. The body and brain begin to operate as though the threat is ongoing, even when it is not. This is why individuals who have experienced trauma may exhibit symptoms such as hypervigilance, heightened startle response, and/or emotional reactivity. This reflects a nervous system that has adapted to prioritize survival in an environment where safety could not be reliably assumed.
When this pattern of neural imbalance and chronic activation persists over time, it can contribute to the development of post-traumatic stress disorder (PTSD). In PTSD, the brain’s survival systems remain over-engaged, while the regions responsible for regulation and contextual understanding struggle to regain control. The heightened reactivity of the amygdala, combined with reduced regulatory input from the prefrontal cortex and impaired contextual processing by the hippocampus, creates a state in which the individual is continually scanning for danger and responding as though a threat is imminent. Because these responses have been reinforced through repeated activation, they become deeply ingrained and automatic, making them difficult to consciously override. As a result, symptoms such as hypervigilance, exaggerated startle response, emotional reactivity, and intrusive memories are not simply reactions to current circumstances, but manifestations of a nervous system that has learned to function in a state of persistent threat. In this way, PTSD reflects not a failure of coping, but an adaptation of the brain and body to experiences in which survival required constant readiness and rapid response.